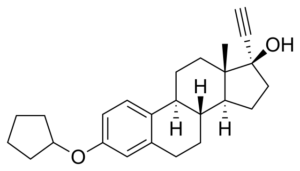
Quinestrol is a synthetic estrogenic compound used in hormone replacement therapy (HRT) for the management of symptoms associated with menopause, including hot flashes, vaginal dryness, and osteoporosis prevention. This comprehensive analysis delves into the origins, mechanisms of action, therapeutic indications, potential side effects, and safety considerations associated with quinestrol.
Origins and Evolution:
Quinestrol was developed in the mid-20th century as a derivative of estradiol, a natural estrogen hormone produced by the ovaries. It was designed to mimic the biological effects of endogenous estrogen while offering improved pharmacokinetic properties and reduced metabolic conversion. Since its introduction, quinestrol has been utilized in HRT regimens to alleviate menopausal symptoms and mitigate the long-term consequences of estrogen deficiency.
Mechanism of Action:
Quinestrol exerts its pharmacological effects by binding to and activating estrogen receptors in target tissues, including the hypothalamus, pituitary gland, uterus, and bones. Through this mechanism, quinestrol restores estrogen levels in postmenopausal women, leading to the alleviation of vasomotor symptoms, improvement of vaginal and genitourinary health, and preservation of bone density.
Key actions of quinestrol include modulation of neuroendocrine function, stimulation of vaginal epithelial proliferation and lubrication, and enhancement of calcium absorption and bone mineralization. Additionally, quinestrol may exert cardioprotective effects by favorably influencing lipid profiles, endothelial function, and vascular tone.
Therapeutic Indications:
Quinestrol is indicated for the management of menopausal symptoms, including hot flashes, night sweats, vaginal dryness, and dyspareunia, as well as for the prevention of osteoporosis in postmenopausal women at risk of bone loss. It is typically prescribed as part of a combination HRT regimen, which may include progestogens to protect the endometrium in women with an intact uterus.
The choice of quinestrol in HRT depends on various factors, including the severity and nature of menopausal symptoms, patient preferences, medical history, and risk factors for cardiovascular disease and osteoporosis. Healthcare providers may tailor HRT regimens to individual patient needs, balancing the benefits of symptom relief and bone protection against the potential risks associated with estrogen therapy.
Potential Side Effects and Safety Considerations:
While generally well-tolerated when used as prescribed, quinestrol is associated with potential side effects and safety considerations, particularly related to its estrogenic properties and systemic effects. Common adverse effects include breast tenderness, uterine bleeding, fluid retention, and mood changes, which may occur due to estrogen stimulation of target tissues.
Of particular concern are the risks of venous thromboembolism, stroke, cardiovascular events, breast cancer, and endometrial hyperplasia, which may be increased with long-term or high-dose estrogen therapy. Patients using quinestrol should undergo regular monitoring of blood pressure, lipid levels, mammography, and gynecological examinations to detect and manage potential adverse effects promptly.
How to Use Quinestrol:
Quinestrol is administered orally as tablets, with dosing tailored to the specific indication and patient characteristics. The recommended starting dose varies depending on the severity of menopausal symptoms, bone density status, and individual response to estrogen therapy. Healthcare providers may initiate quinestrol therapy at a low dose and titrate gradually based on treatment response and tolerability.
Patients should be counseled on proper medication use, including the importance of adherence to HRT regimens, regular follow-up visits, and monitoring of treatment response and side effects. Healthcare providers may consider alternative formulations, routes of administration, or combination therapies to optimize symptom relief and minimize the risk of adverse outcomes in individual patients.
Conclusion:
Quinestrol remains a valuable therapeutic option for the management of menopausal symptoms and osteoporosis prevention in postmenopausal women, offering significant benefits in terms of symptom relief, genitourinary health, and bone protection. Its well-established efficacy, safety profile, and availability in oral formulations make it a preferred choice for many patients and healthcare providers.
However, the use of quinestrol necessitates careful consideration of potential side effects, safety concerns, and individual patient factors. Healthcare providers play a crucial role in patient education, dose optimization, and monitoring to ensure safe and effective use of quinestrol while minimizing the risk of adverse effects and complications. Close collaboration between patients, caregivers, and healthcare providers is essential to optimize treatment outcomes and promote women's health during the menopausal transition and beyond.