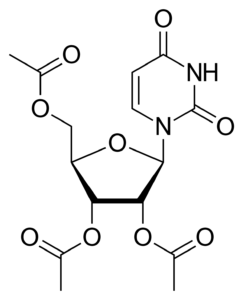
Uridine triacetate, a pyrimidine analog, has emerged as a valuable therapeutic agent in the management of toxicities associated with fluoropyrimidine chemotherapy. This comprehensive review aims to elucidate its origins, mechanisms of action, therapeutic indications, potential side effects, and safety considerations.
Origins and Evolution:
Uridine triacetate was developed as an antidote to counteract severe toxicities induced by fluoropyrimidine chemotherapy agents, such as 5-fluorouracil (5-FU) and capecitabine. Initially synthesized in the late 20th century, uridine triacetate gained approval from regulatory agencies as a critical intervention for the prevention and treatment of life-threatening fluoropyrimidine-associated toxicities, such as severe gastrointestinal mucositis and hematologic complications.
Mechanism of Action:
Uridine triacetate exerts its therapeutic effects through multiple mechanisms, primarily involving the restoration of depleted pyrimidine pools and inhibition of further incorporation of toxic metabolites into RNA and DNA. By serving as a substrate for uridine kinase and cytidine deaminase, uridine triacetate facilitates the replenishment of intracellular uridine levels, thereby mitigating the deleterious effects of fluoropyrimidine toxicity on rapidly proliferating tissues and cellular processes.
Moreover, uridine triacetate competes with toxic fluoropyrimidine metabolites for incorporation into RNA and DNA, effectively blocking their incorporation and preventing downstream cytotoxic effects. This dual mechanism of action underpins the protective and therapeutic effects of uridine triacetate in mitigating fluoropyrimidine-induced toxicities and improving patient outcomes.
Therapeutic Indications:
Uridine triacetate is indicated for the emergency treatment of adult and pediatric patients with life-threatening or severe toxicities following the administration of fluoropyrimidine chemotherapy agents, such as 5-fluorouracil (5-FU) or capecitabine. Its rapid onset of action and ability to mitigate gastrointestinal mucositis, myelosuppression, and other severe adverse effects make uridine triacetate a critical intervention in the management of fluoropyrimidine-related toxicities, potentially saving lives and improving treatment tolerability.
Potential Side Effects and Safety Considerations:
While generally well-tolerated, uridine triacetate may be associated with potential side effects and safety considerations, including gastrointestinal disturbances, nausea, vomiting, and diarrhea, which may occur transiently during treatment initiation or administration. However, the overall safety profile of uridine triacetate is favorable, with few serious adverse events reported in clinical trials and post-marketing surveillance.
Notably, uridine triacetate is contraindicated in patients with a known hypersensitivity to uridine triacetate or any of its components, as well as in individuals with hereditary fructose intolerance due to the presence of sorbitol in the oral suspension formulation. Special precautions should be taken in patients with preexisting renal impairment or electrolyte abnormalities, with close monitoring of renal function and electrolyte levels recommended during uridine triacetate therapy.
How to Use Uridine Triacetate:
The dosing and administration of uridine triacetate are contingent on the severity of fluoropyrimidine-associated toxicities, patient age, weight, renal function, and clinical status. Uridine triacetate is typically administered orally as an oral suspension or powder for reconstitution, with dosages calculated based on body surface area and the specific toxicities requiring treatment.
For adults and pediatric patients weighing 10 kilograms (kg) or more, the recommended dosage of uridine triacetate is 10 grams (g) every 6 hours for 20 doses, administered orally as soon as possible following the onset of severe or life-threatening fluoropyrimidine-associated toxicities. For pediatric patients weighing less than 10 kg, the dosage is calculated based on body surface area and administered at a dose of 6.2 mL/m² every 6 hours for 20 doses.
Patients should be counseled on the importance of adherence to prescribed dosing regimens, completion of the full course of treatment, and reporting of any adverse effects or concerns to healthcare providers promptly. Close monitoring of clinical status, laboratory parameters, and treatment response is essential to ensure optimal outcomes and mitigate the risk of treatment-related complications.
Conclusion:
Uridine triacetate represents a critical intervention in the management of severe or life-threatening toxicities associated with fluoropyrimidine chemotherapy, offering rapid reversal of adverse effects and potentially saving lives in oncology patients. Its mechanisms of action, therapeutic indications, and safety considerations underscore its significance as a cornerstone therapy in the armamentarium of oncologists, pharmacists, and healthcare providers.
However, the use of uridine triacetate necessitates careful consideration of potential side effects, contraindications, and individual patient factors. Healthcare providers play a pivotal role in patient assessment, treatment decision-making, and therapeutic monitoring to ensure safe and effective utilization of uridine triacetate while optimizing treatment outcomes and promoting patient well-being.
Collaborative efforts between oncology teams, supportive care providers, and pharmacists are essential to facilitate timely access to uridine triacetate, educate patients and caregivers about its appropriate use and safety profile, and implement proactive measures to prevent and manage potential adverse effects or complications. By leveraging its cytoprotective and antidotal properties, uridine triacetate continues to play a vital role in safeguarding oncology patients from the debilitating effects of fluoropyrimidine-associated toxicities, enhancing treatment tolerability, and improving overall quality of life.